Home » Telemedicine connects Tri-City patients to specialists
Telemedicine connects Tri-City patients to specialists
August 15, 2019
Virtual doctor’s visits becoming more widely available – not just for routine illnesses
Tri-City
patients are connecting with medical specialists for more types of care, thanks
to the growing use of telemedicine, or telehealth, which can allow a provider
to make some diagnoses of a critical patient without even being in the same
room.
“Telehealth
started as an access strategy to improve access to care in communities where
patients wouldn’t otherwise have that and really it was around specialists to
start,” said Dr. Todd Czartoski, a neurologist and chief executive of
telehealth for Providence St. Joseph’s Health, the parent company of Kadlec
Regional Medical Center in Richland.
In
the 12 years since the hospital network first incorporated telemedicine into
its practices, the fields have grown to include stroke detection, Lou Gehrig’s
disease treatment, speech therapy, psychiatry, dietetics, maternal fetal
medicine, wound care and genetic counseling. These specialties are in addition
to the Express Care service offered for diagnosis of routine illnesses like
strep throat, ear infections or pink eye. These are options available to
patients using their own device to connect with a provider.
“You
could be anywhere. You could be sitting in your home or car. It’s incredibly
convenient,” said Cassandra Bilodeau, a registered nurse and director of outreach
and development for telemedicine at Providence.
For
conditions that require a specialist, patients would be seen by a provider at a
clinic or hospital using a high-tech cart, which puts the clinician virtually
in the room with a patient, similar to Skype or FaceTime, while remaining
compliant with federal privacy laws to protect patients’ medical information.
The telemedicine effort through Providence started with stroke diagnosis by
keeping a stroke neurologist on call at all times to assess patients during the
crucial initial minutes when it’s suspected someone may have suffered a
cerebrovascular accident.
“When
Dr. Czartoski logs in to the software, we see his face pop up and there’s a
nurse in with the patient because this is a
critical patient and you need medical personnel there to attend to them,” said
Abigail Richardson, a registered nurse and telemedicine coordinator at
Providence. With the help of a trained telepresenter, “You’re helping the
physician finish the exam, so you’re testing for arm and leg weakness and those
types of things, visual deficits. And then Dr. Czartoski, on his end, can make
the assessment, how we’re going to treat this.”
By using telemedicine, the hospital can leverage its
expertise to get patients the necessary care or diagnosis as quickly as
possible.
“We like to call it moving knowledge, not people,”
Czartoski said. This allows two stroke-trained neurologists to serve 55
hospitals across the Providence St. Joseph system.
“When you think about 50 hospitals it sounds like an awful
lot, and it is, so we’ve had redundancy and backup built in for what we call
the ‘jump ball’ model, and that’s been super helpful for the backup so we have
quick responsiveness,” Czartoski said. “Our responsiveness 24 hours a day is
two minutes, two seconds. That’s our average time it takes to get an answer
from a stroke neurologist when they’re paged.”
For some patients, the speed of seeing a provider isn’t
critical, but rather a matter of convenience. Some patients appreciate the
ability to see a specialist without traveling outside the region.
This is the case for patients with amyotrophic lateral
sclerosis, known as ALS, or Lou Gehrig’s disease. Prior to the use of
telemedicine, patients often had to travel to Spokane or Seattle to see a specialist
in the field.
“These caregivers that are helping out have a huge burden
for them to be able to travel the patient over the mountains,” Bilodeau said.
“We have wrap-around service where it’s very comprehensive with all of our
ancillary services with a neurologist able to come in and see these patients
and keep them local. So it decreases the burden for the family.”
A visit with a patient diagnosed with ALS tends to last
about three hours using a multi-disciplinary approach. The virtual visits are
done only after the patient has had an in-person visit with an expert in
Seattle who offers the initial establishment of care and diagnosis.
“When they’re coming here, they have those direct
caregivers in the clinic who go in teams,” said Lisa Braudrick, supervisor of
therapy services. “One of the teams is comprised of the neurologist who’s on
the cart, and then there’s the nurse in the room, as well as the respiratory
therapist. So the nurse and the respiratory therapist might be doing hands-on
with the patient, but the neurologist is also asking and getting an idea of
what’s going on and what are the concerns.” The Kadlec team said telehealth can
really mirror what could be done entirely in person.
While telemedicine can allow patients in the Tri-Cities to
be seen by specialists outside the area, it also offers the same opportunities
in reverse, bringing local experts to more remote locations around the region
and as far away as Montana, using the Providence network.
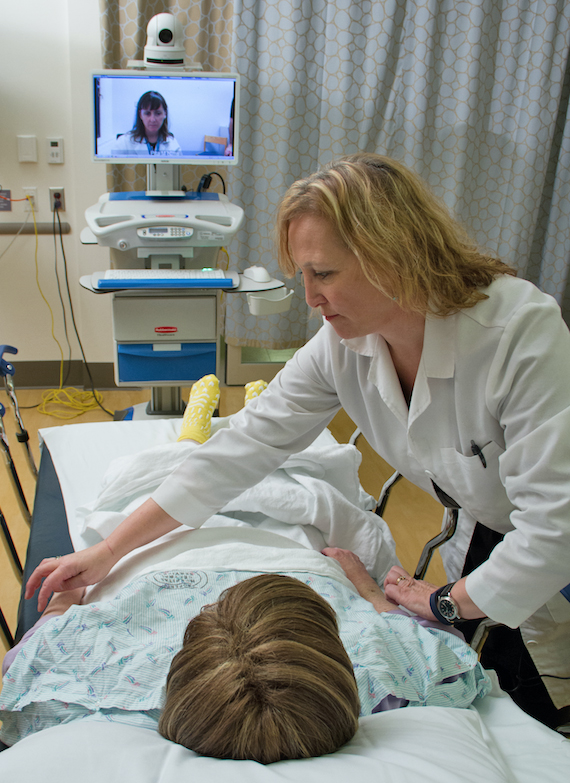
“There are communities where we simply don’t have that
ability to have a provider there each and every day,” Czartoski said. “The way
I’ve described it more recently is, we’re essentially following in the
footsteps of what some of the tech companies have done, like Microsoft and
Amazon and Google, we’re building on a cloud. They built this cloud
infrastructure that would allow you to only purchase the amount of server space
that you needed instead of investing in an entire server farm with computer
hardware. We’re building a clinical cloud that allows you to use and access
world experts in different areas without investing in an entire team of stroke
neurologists or psychologists or intensivists.”
After more than a decade of building on this model, there
remains a question of how else telemedicine can be leveraged to assist
patients.
“There’s a few services that make sense to scale because
we’re never going to have enough stroke specialists and psychiatrists,” said
Czartoski, who described what he calls the “secret sauce for success.”
“When we vet new opportunities, the lens that our team
uses, we really ask four questions: one, first and foremost, can we provide
care safely doing it remotely using telehealth? And if you can’t answer that without
certainty, we stop there.”
When the team is confident the care can be provided
safely, the next assurance is whether it can be offered with high quality.
Czartoski said. “Is the quality of service and care that we’re delivering
better or as good as we would be able to do with an in-person service? In some
cases that means stroke care to an outlying facility where we don’t have any
stroke neurologists available, having a stoke neurologist available by video is
actually better than the status quo.”
The team also assesses whether the financial model for a
new telemedicine setup will be sustainable.
“We can get grants for telehealth, but if it’s not built
in a way that allows us to at least cover the cost of the program, our
experience has been that you won’t get it to take off and spread in scale and
be used as much as we would want,” said Czartoski, who says the final piece of
the “secret sauce” recipe includes a “provider champion” who believes in the
system. Someone who will, “wake up every day and think, ‘I’m going to make this
a successful telehealth program,’ ” said Czartoski.
The telemedicine option also is beneficial to fill gaps in
service, either due to a lack of demand or the time between recruiting a new
provider. This includes speech therapy, which can be a game-changer for rural
communities where there aren’t enough patients to warrant a provider on staff
full time.
“It’s like the cloud model where they’re paying when they
need it because they don’t need it full-time,” Bilodeau said. “It’s also hard
for them to recruit specialists when someone leaves. Rather than go months and
months, and having that gap, we’re looking at telemedicine to help meet the
need.”
The team said starting up a new telemedicine offering is
not as simple as just supplying a cart. “It’s like setting up a new clinic, if
you will. It takes a lot to vet it and ensure that we’re doing it correctly,”
Bilodeau said.
Kadlec sees telehealth services as an increase to the care
that’s available and not a means of replacing true face-to-face contact between
a provider and patient.
“It’s enhancing it and allowing us to meet the patient
where they need to be met,” Bilodeau said. “I think the options really are
endless and that’s scary for a lot of people, but I think we really need to
think outside the box because telemedicine can really help our communities, our
patients, and when you look at the social determinates of health and why people
can’t get access to care, telemedicine can really help mitigate all those
challenges. It can help reduce barriers.”
Bilodeau said a patient or provider always has the option
of requesting an in-person visit if either party feels they cannot capture what
needs to be captured using a virtual appointment. But, she added, it has never
happened.
Trios Health in Kennewick uses telemedicine through its
Urgent eCare service for diagnosis of minor illnesses.
Media contacts for Trios and Lourdes
Health did not immediately return requests for more information on their
telemedicine offerings. Both hospitals are owned by Tennessee-based LifePoint
Health.
Local News Science & Technology
KEYWORDS august 2019